We asked our social media followers for their top questions on contraception. To mark World Contraception Day, MSI UK’s Lead Contraception Nurse, Julia Hogan, answers them for you.
Here are Julia’s answers to six of your most commonly asked questions on all things contraception:
“I keep forgetting to take my combined pill every day, are there any other similar methods I can use?”
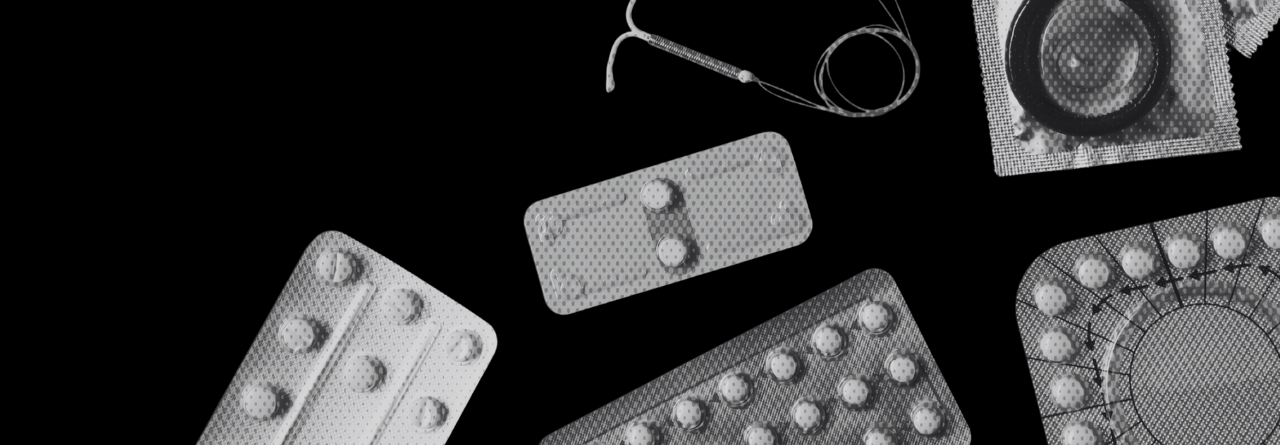
Yes! A lot of people that I see in my practice are only aware of the contraceptive pill, as this is the most popular method in the UK, but there are other methods of contraception that use the same hormones as the combined contraceptive pill and are just as effective. You could try either the vaginal ring, which stays inside the vagina for three weeks, or the contraceptive patch, which you replace weekly before having a week without a patch.
However, if you’re really struggling to remember your pill, and think you’d find replacing a patch or vaginal ring inconvenient, you could try a long-acting reversible method (LARC). LARC methods include the implant, injectables, and Intrauterine Contraception (also known as coils). Depending on the brand, injectables protect you against pregnancy for between 8 and 13 weeks, and the implant provides you with continuous protection against pregnancy for 3 years. The coils, depending on which one you choose, can protect against pregnancy for between 3 and 10 years.
“Is there a chance using contraception could affect my fertility if used for a long time?”
No – all the evidence shows that contraception has no effect on your long-term fertility whatsoever, and your fertility will return to normal within two weeks after you stop taking the pill or have an implant or IUD removed. The only method where your fertility can be slow to return after stopping is the injection, as it can take an average of 6 months for fertility to return to normal.
“I’ve heard that the pill can make you gain weight and can cause cancer – is this true?”
There’s no clear evidence that weight gain is associated with the contraceptive pill and taking hormonal contraception can help your body in many ways. Being in control of your fertility can have a positive impact on your mental health, as well as physical benefits such as regulating your bleeding, reducing period cramps, and improving your skin. The combined hormonal pill can also help women going through the menopause, or experiencing peri-menopausal symptoms, by reducing side effects such as hot flushes. There’s also evidence that it can help protect against bone loss (a side effect of the menopause caused by the drop in oestrogen levels) up until the age of 50.
In regards to cancer risk, there are some studies that indicate a very small increased risk for women taking the contraceptive pill for cervical and breast cancer, but this risk declines over time once women have stopped taking it. There are also studies that show that women taking the pill have a reduced risk of developing ovarian, colorectal and endometrial cancers.
“I don’t want to be on hormonal contraception anymore – what methods of non-hormonal contraception are available?”
I am meeting lots of women who are keen to have a non-hormonal method and I always talk about the benefits on the copper coil. The copper IUD is a small, T-shaped device that’s put into your uterus by a doctor or nurse. The copper alters the cervical mucus, which makes it more difficult for sperm to reach an egg and survive in the womb. It can also stop a fertilised egg from being able to implant. When inserted correctly, it’s more than 99% effective and can last for 5 to 10 years, depending on the type. For the first sixth months after getting an IUD fitted, you may experience heavier, longer, or more painful periods but this usually settles in time.
“What’s it like having a coil inserted… is it as painful as everyone says?”
Having intrauterine contraception (IUC) fitted may be uncomfortable or painful, but the whole process should only take around five minutes and we use some local anaesthetic to ease the process. It involves inserting a speculum (an instrument that holds open the walls of the vagina so that the neck of the womb can be seen), which is the same instrument that is used when a smear test is taken. This can be uncomfortable for some women, but not painful. Forceps are then used to hold the cervix steady, which can cause a little pain that settles after a few minutes, and a probe is then used to measure the length of the uterus to check how the IUC should be inserted. At this point, you may experience period-type pain. Then, the IUC is inserted in a narrow tube with the arms folded down. As it reaches the top, or neck, of the womb, it can cause period-type pain again, but this should stop once its in place, and then the tube, forceps, and speculum are removed. People normally experience cramping afterwards, but this should pass after a few minutes. Some women, particularly those who have given birth vaginally, say the process is pain-free, but it always depends on the individual. Your provider will talk you through the process beforehand and will be able to answer any questions you may have.
“Will there ever be a male contraceptive?”
Currently, the only readily available method of contraception for men is the condom or vasectomy. Vasectomy is a popular permanent method of contraception chosen by millions of men worldwide. It’s completely safe and is one of the most effective methods of contraception that exists. The procedure takes about 15 minutes and does not affect your hormones, orgasm, or ejaculation, so there’s no reason why a vasectomy should affect sex life.
Learn more about contraception in our explainer – Contraception Explained.