
Latest
25 March 2026 | 7 min read
Impact
50 years of MSI
Stories and impact from MSI Reproductive Choices’ 50 years of delivering reproductive choice for women and girls.
Story

Explore the latest
Topics
All
Abortion
Adolescents
Contraception
Crisis settings
Digital health
Gender equality
Health systems
Impact
Leave no one behind
Policy and advocacy
Quality
Self-managed health
Types
All
Campaign
Explainer
News
Opinion
Other
Press release
Research
Resource
SafeAccess
Story
Webinar
Explore the latest
Latest posts
News

21 May 2026 | 2 min read
Policy and advocacy
Statement on UK government’s new international effort to drive progress for women and girls
MSI statement on the UK government’s new International Strategic Framework on Women and Girls, and a new International ...
News

20 May 2026 | 1 min read
AbortionPolicy and advocacy
Statement on study showing that U.S. abortion bans restrict miscarriage care
MSI statement on a new study finding that abortion bans in the US are restricting miscarriage care.
News
15 May 2026 | 4 min read
AbortionPolicy and advocacy
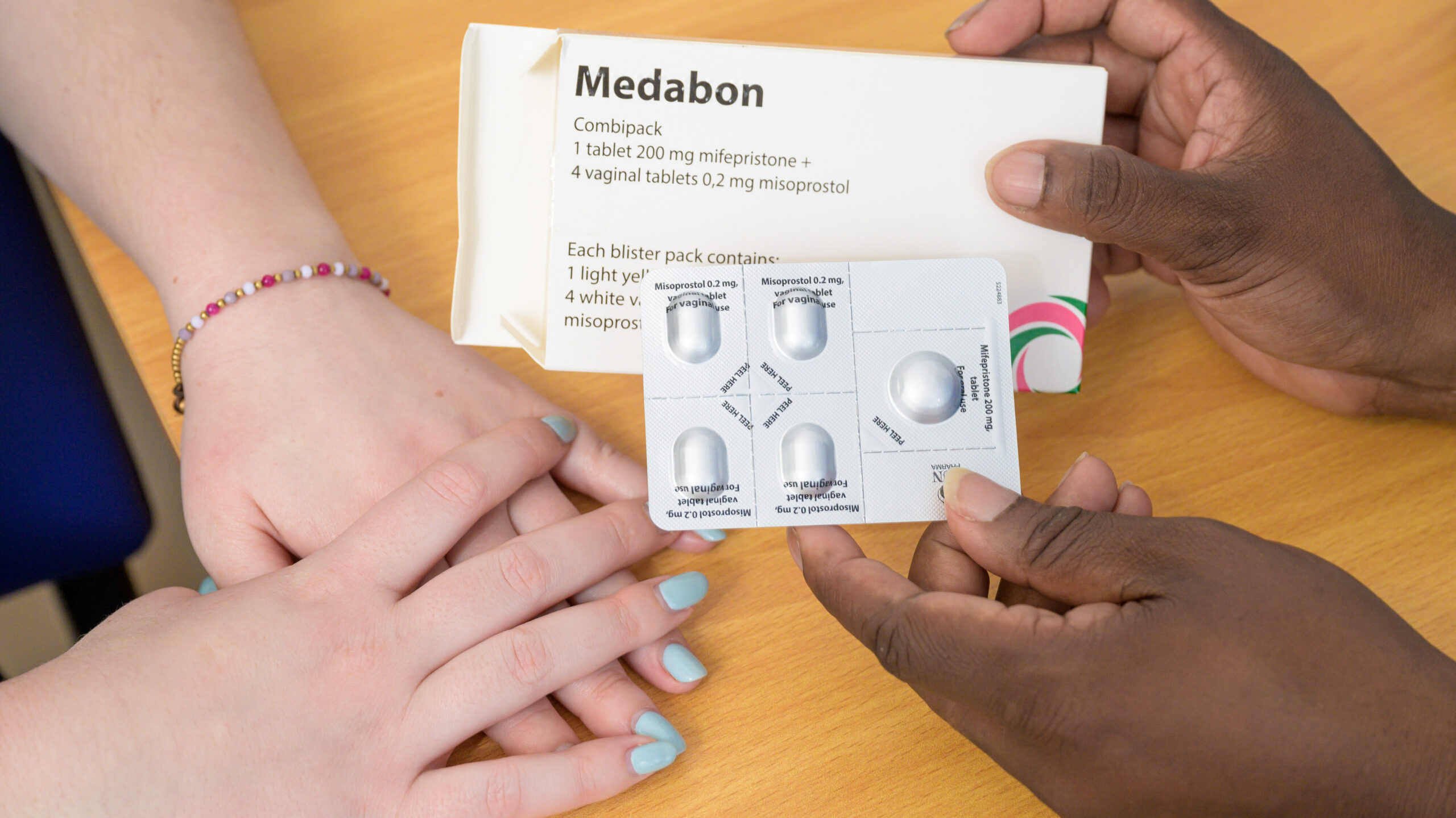
MSI statement on U.S. legal actions to restrict access to mifepristone
A recent U.S. federal court ruling restricting access to mifepristone is not grounded in medical evidence and fuels ...
Story

6 May 2026 | 12 min read
Impact
The inventive, whirlwind early years of MSI – as told by first team members
It’s 1976. Meet Kim Lavely and Douglas Whitewright: two team members at MSI’s first clinic in London.
Story

29 April 2026 | 5 min read
ContraceptionLeave no one behind
Anna’s story: Supporting women in Sierra Leone through war, Ebola and more
Anna, a long-serving team member, shares how MSI Sierra Leone has persevered against the odds.
Campaign

15 April 2026 | 5 min read
ContraceptionImpact
Invest in a lifetime
Cost-effective, transformational, social impact. Here’s our pitch for the investment of a lifetime.
News
30 March 2026 | 2 min read
ContraceptionPolicy and advocacy
Statement on the reported waste of $9.7 million worth of USAID contraception
MSI statement on reports in the New York Times that $9.7m worth of USAID contraception has been left in a warehouse and ...
Story

25 March 2026 | 7 min read
Impact
50 years of MSI
Stories and impact from MSI Reproductive Choices’ 50 years of delivering reproductive choice for women and girls.
Story

25 March 2026 | 6 min read
Contraception
Mohsina: A trailblazer for women and girls in Pakistan
Dr Mohsina Bilgrami set up a reproductive healthcare programme in Pakistan. She has a fascinating and historied story to ...





