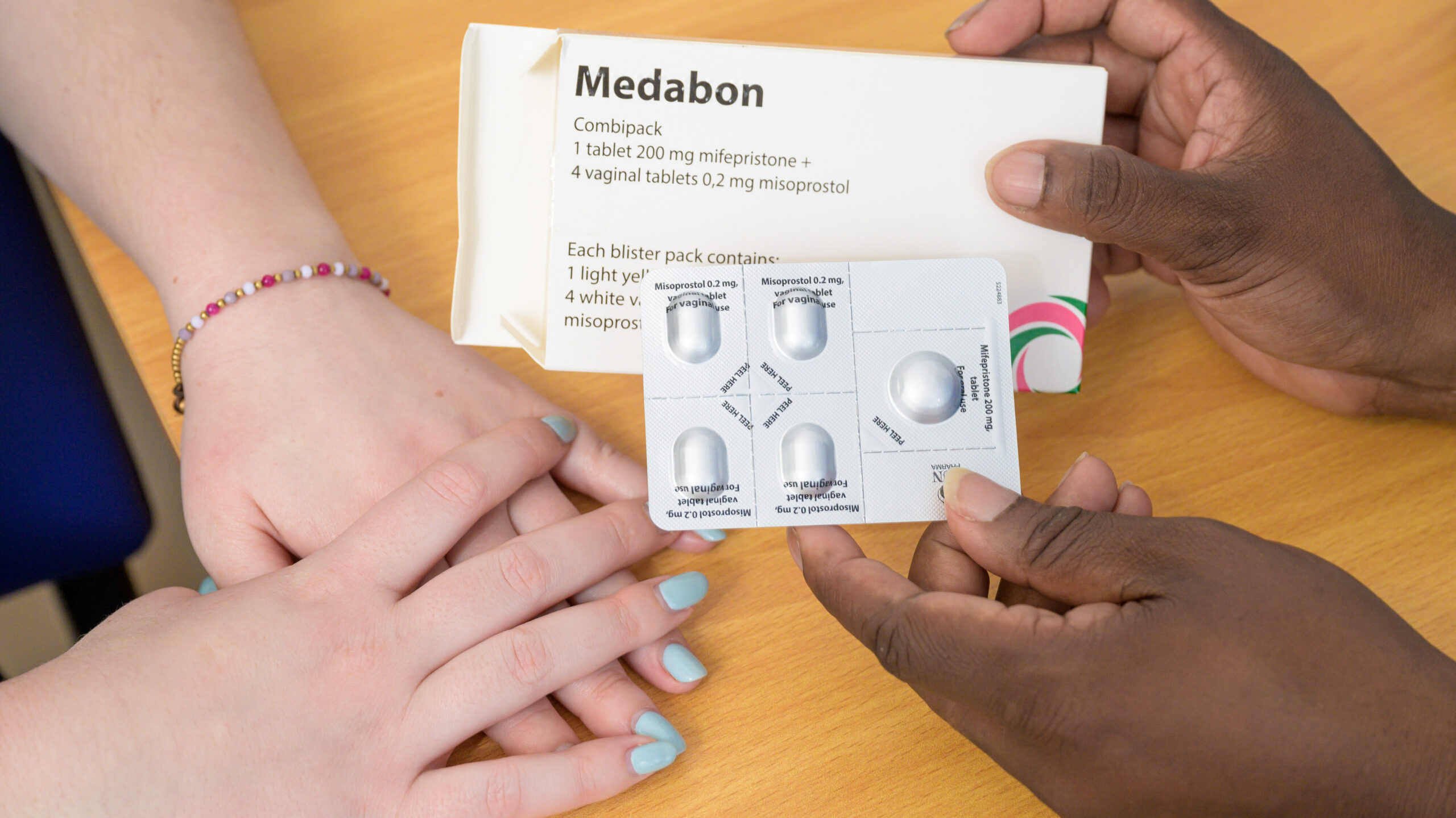
What does SRHR mean?
SRHR stands for sexual and reproductive health and rights. Sexual and reproductive health can be defined as a person’s right to a healthy body – the autonomy, education and healthcare to freely decide who to have sex with, and the knowledge and health products to avoid sexually transmitted infections or unintended pregnancy. Sexual health is an integral part of overall health and wellbeing, ensuring people can have pleasurable and safe sexual experiences, free of coercion, discrimination or health risks.
Access to sexual and reproductive health services enable people to exercise this right. Sexual and reproductive healthcare can take the form of medical care related to the reproductive system, for example, to treat a sexually transmitted infection, or services that support reproductive choice with the provision of contraception and abortion care.
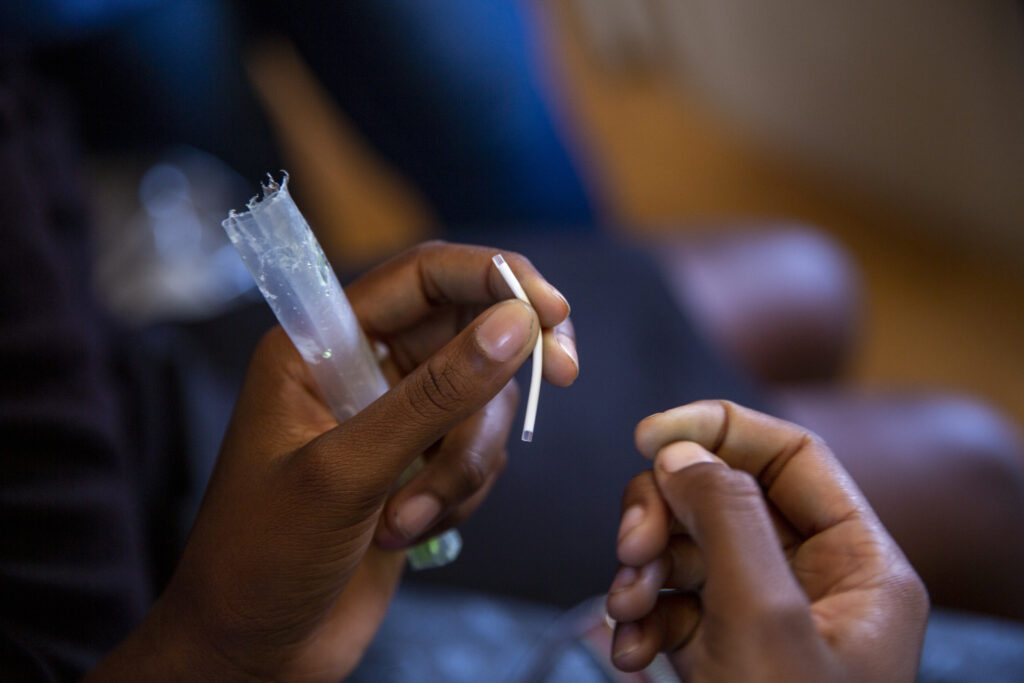
Supporting sexual and reproductive health with contraception
Access to contraception is a central component of sexual and reproductive healthcare. Contraception gives people autonomy over their reproductive health with the ability to decide if, or when, they would like to become pregnant.
By offering a choice of contraceptive methods, sexual and reproductive healthcare providers enable people to make informed decisions about their future fertility. By choosing an IUD, for example, a woman can prevent pregnancy for up to 12 years, or, by opting for a barrier method such as the condom, they can prevent pregnancy for a shorter period, as well as protect against sexually transmitted infections.
The ability to choose if or when to become pregnant can have a far-reaching impact on an individual’s ability to make other life decisions. With reproductive choice, people can determine their own futures, for example, by choosing to stay in education or pursue their career.
But not everyone who wants contraception is able to access it. Currently, across low- and middle-income countries, there are 257 million people with an unmet need for contraception. This lack of access is having a devastating impact on lives and futures.
MSI’s analysis found that every year, across sub-Saharan Africa, up to 4 million girls drop out of school or are excluded due to teenage pregnancy. Universal access to contraception can not only advance people’s sexual and reproductive health, but can also help reverse one of the main perpetuators of inequality: girls’ lack of access to education.
“At school, we often see girls become pregnant. Usually they don’t come back.”
Aisha*, pictured right, is a young Senegalese woman in her late teens. Last year, she accessed contraception with MSI Senegal.
When we spoke with her, she had just been able to finish her final year of school. “It’s thanks to MSI that I was able to finish my studies,” she told us. “If MSI wasn’t here I don’t know what my life would be like today.”
When girls like Aisha can access quality education, they are better able to pursue a career, create opportunities in their communities and drive positive change in wider societies.

Women’s access to safe abortion
Women will always need access to abortion. No form of contraception is 100% effective and across the world, almost 1 in 3 pregnancies end in abortion, with millions of people deciding to have an abortion every year.
Laws that govern abortion access vary from country to country. This means that women’s access to safe abortion depends largely on where they live. For example, in the Philippines and El Salvador, abortion is prohibited in all circumstances, whereas in Sweden, abortion care is available on request up to 18 weeks of gestation.
Making abortion more legally restricted does not stop people from requiring abortions. Data from the Guttmacher Institute shows that abortion rates are similar in countries where abortion is broadly legally accessible and those where it is restricted. What varies is that in countries where abortion is more restricted, the number of women dying due to unsafe abortion rises. This shows that rather than reducing the number of abortions taking place, restricting women’s access to abortion results in more women seeking unsafe – in some cases fatal – services instead.
Unsafe abortion puts the health and lives of women at risk. Currently, almost half of all abortions that take place worldwide are unsafe: an estimated 35 million each year. As a result, seven million women face health complications, and over 22,800 lose their lives.
But it’s not just legal restrictions that force women to turn to unsafe abortion. Harmful cultural norms, a lack of access to accurate information, and inaccessible or poorly funded reproductive healthcare services contribute to women seeking an abortion that is less safe. If we are to end unsafe abortion for good, we must ensure that women’s access to safe abortion is not only supported by policy, but that it is de-stigmatised, adequately funded, and easy to access.

“I know I’m doing the right thing and that this job is saving lives.”
Toch, pictured left, is an abortion provider for MSI in Cambodia.
“I love what I do because I know that it is saving lives.
“But many people are still too shy to talk about abortion because it’s seen as a shameful subject.
“When women are unable to talk openly about their health, it can have serious consequences. When we talk about it openly and women feel educated about their reproductive health, they can find a safe place to have an abortion.”
Societal stigma
Societal stigma around sexual and reproductive health and rights is one of the ways a person’s access can be restricted.
Harmful cultural norms such as beliefs that only some people should access sexual and reproductive health services, perpetuate stigma, driving misinformation and in some cases, fear, shame, and intimidation among people seeking healthcare. Stigma can also impact the willingness of providers to offer services, and can prevent groups, such as adolescents, from being able to access information on the options available to them.
MSI’s research in the UK revealed that just one in three women in the UK would tell their family if they were considering abortion, proving the wall of silence that exists around abortion care even in a country where abortion is legally unrestricted. Our My Body, My Voice report also revealed that nearly one in four of MSI’s abortion clients (23.4%) across Latin America, Africa, and Asia reported experiencing some form of stigma from their partner, their community and in some cases, sexual and reproductive healthcare providers.
Societal stigma can have devastating consequences. When people are forced to prioritise secrecy, they’re more likely to seek unsafe sexual and reproductive health services that put their lives and futures at risk.
By being open about sexual and reproductive health, we can help dismantle the societal stigma around contraception and abortion care. Sharing your story can be an effective way of making people feel less alone in their choices and can help increase awareness around the necessity of sexual and reproductive healthcare, including contraception and abortion care.
“If you empower a woman or a girl, then you’ve empowered a home, you’ve empowered a country and you’ve empowered the world.”
Damaless – Nurse, MSI Zambia
Why sexual and reproductive health matters
Sexual and reproductive health matters because it is an essential component of an individual’s overall health and wellbeing. It’s important – and a human right – for people to have the right to health, to be free from sexual violence and to determine whether to become pregnant.
Evidence shows that by supporting girls to access an education, we can reduce inequality and break cycles of poverty. When young women gain access to contraception, it increases their enrolment in higher education. Each additional year of education can increase a woman’s earnings by up to 20%, which would contribute to closing the gender pay gap and could boost global GDP by $28 trillion.
When sexual and reproductive health needs and rights are met, individuals can make choices about their own bodies and futures, which can have a knock-on impact on their families’ welfare and future generations. And because it is often women who face the health and financial implications of not having access to services like contraception and abortion care, sexual and reproductive health and rights is key to advancing gender equality.
Education and reproductive choice
By enabling girls to stay in school, sexual and reproductive health and rights has a crucial role to play in advancing gender equality.
But currently, millions of girls are out of school. Research from the Population Council across six Sub-Saharan African countries found that nearly all adolescent girls who have ever been pregnant are no longer in school, with 1 in 4 girls in Malawi dropping out of school for this reason.
The evidence clearly shows that education and reproductive choice are linked. By supporting adolescents’ sexual and reproductive health and rights, we can help girls to stay in school, complete their education, and contribute to a fairer world for all.
How does MSI support sexual and reproductive health?
MSI Reproductive Choices has been providing sexual and reproductive healthcare services for 50 years.
Our teams work across 36 countries to support over 94,000 people every day to make choices about their reproductive health and futures. We provide contraception, comprehensive abortion care, and maternal healthcare services wherever they’re needed – from major cities to rural, hard-to-reach villages.
MSI’s centres and maternity hospitals offer a range of reproductive healthcare services supporting women throughout their lives, as their bodies and needs change.
Sexual and reproductive healthcare is a proven ‘best-buy’ in international development. We are proud of the impact we have made so far, reaching more than 200 million women worldwide since 1976. But we know our job is far from done. We’re working to deliver on a bold, but simple, vision that by 2030, no abortion will be unsafe and every individual who wants access to contraception will have it.
With your help, we can go further.
Join us in making choice a reality for everyone
Reproductive choice changes lives. Together, we can make choice possible.

Donate to reproductive choice
It costs only £6 per year – or 2 pence per day – for MSI to provide someone with life-changing sexual and reproductive healthcare, giving them the power to decide if or when to become pregnant.
Subscribe for email updates
By subscribing for email updates and joining our community of reproductive choice advocates you can stay up-to-date with the latest news and campaigns on reproductive healthcare and rights.

Partner with us
Whether you give time, money, or expertise, your investment could benefit women and families for generations to come. Want to join our vision and help us make choice a reality for everyone?